Uveitis is a condition where the uvea becomes inflamed. The uvea includes three structures in the eye: the iris (colored part of the eye), ciliary body (fluid producing structure), and choroid (structure that nourishes the retina). Uveitis can be classified into three types. Anterior uveitis is the inflammation of the anterior uvea (iris and ciliary body). Posterior uveitis is the inflammation of the posterior uvea (choroid). Panuveitis is the inflammation of both the anterior and posterior uvea.
Clinical signs of anterior uveltis include hyphema (blood in the eye), aqueous flare (cloudiness of the front part of the eye due to inflammatory cells), a thickened and discolored iris, hypotony (decreased intraocular pressure), miosis (constricted pupil), and corneal edema. Clinical signs of posterior uveltis include decreased vision and retinal detachment. Patients with uveitis sometimes show excessive lacrimation(tearing), and photophobia (fear of light).
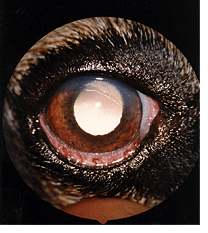
Uveitis is not a disease, but a symptom of another condition. There are many disorders that cause uveitis, and they can be classified into two groups. These are exogenous (external to the eye) causes, such as trauma to the eye or corneal ulceration, and endogenous (within the eye or through the bloodstream to the eye), There are quite a few endogenous causes including bacterial, fungal, and viral infections. Neoplastic, toxic, metabolic, and autoimmune diseases are also a consideration. Steps to determine the cause of uveitis include a thorough history and physical examination, a complete blood count (CBC), blood biochemistry profile, urinalysis, and bacterial and fungal titers.
The ultimate goal in the treatment of uveitis is to treat the clinical signs while at the same time trying to determine its cause. It is very important to treat the clinical signs immediately, even if the primary cause of uveitis is not determined. Prolonged uveitis may result in serious problems including cataract formation, secondary glaucoma, retinal detachment and ultimately blindness. Treatment may include both topical and oral medications, most commonly antibiotics and anti-inflammatory agents. Corticosteroids are the most commonly used anti-inflammatory agents, but these cannot be used in patients with keratoconjunctivitis sicca (dry eye disease) or diabetes. For these patients, non-steroidal anti inflammatory drugs (NSAID’s) are utilized.
ATLANTA VETERINARY EYE CLINIC
33 Avondale Plaza North
Avondale Estates, GA 30002
Map & Directions | Email
OFFICE HOURS
M W F 9:00 am - 3:00 pm
T Th 9:00 am - 6:00 pm
Saturdays Closed
Sun Closed
OFFICE HOURS
CALL TO SCHEDULE AN APPOINTMENT
WE ACCEPT
